0
Publication
Community:
Dec 17, 2018
In response to the heightened interest in the relationship between work and the health of individuals and communities, CMCS has clarified that Medicaid funds cannot be used to pay beneficiaries’ wages, but can pay for employment counseling as an optional benefit—to help people get jobs. Years of experience with work requirements for the Supplemental Nutrition Assistance Program, Aid to Families with Dependent Children, and populations with disabilities have developed the evidence for what is needed to help different populations find and keep jobs.
Authored by: Christopher F. Koller for Millbank Memorial Fund
Topics: Affordable Care Act, Disabilities, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Research, Stability, Workforce development
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Dec 17, 2018
Christopher F. Koller for Millbank Memorial Fund
In response to the heightened interest in the relationship between work and the health of individuals and communities, CMCS has clarified that Medicaid funds cannot be used to pay beneficiaries’ wages, but can pay for employment counseling as an optional benefit—to help people get jobs.
0
Publication
Community:
Dec 14, 2018
Health and reentry are closely related, and chronic medical, mental health, and substance use problems make it harder for newly released people to seek employment, obtain housing, and avoid reincarceration. Compared with the general population, justice-involved people tend to be in poorer health and need access to physical and behavioral health services, as well as the know-how and motivation to get care.
Authored by: Rochisa Shukla and Kamala Mallik-Kane for Urban Institute
Topics: Affordable Care Act, Criminal justice, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Research, Stability
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Dec 14, 2018
Rochisa Shukla and Kamala Mallik-Kane for Urban Institute
Health and reentry are closely related, and chronic medical, mental health, and substance use problems make it harder for newly released people to seek employment, obtain housing, and avoid reincarceration.
0
Case study
Community:
Dec 11, 2018
As the Trump Administration continues to encourage states to take Medicaid coverage away from people who don’t meet a work requirement, a new report describes Montana’s promising alternative: a workforce promotion program that targets state resources toward reducing barriers to work.
Authored by: Hannah Katch for Center on Budget and Policy Priorities
Topics: Affordable Care Act, Asset building, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Partnerships, Research, Workforce development
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Dec 11, 2018
Hannah Katch for Center on Budget and Policy Priorities
As the Trump Administration continues to encourage states to take Medicaid coverage away from people who don’t meet a work requirement, a new report describes Montana’s promising alternative: a workforce promotion program that targets state resources toward reducing barriers to work.
0
Publication
Community:
Dec 6, 2018
The administration has proposed an expansion of the “public charge” rule that would make it more difficult for applicants whom officials deem likely to rely on public assistance to obtain lawful permanent residence (a “green card”) or a temporary visa. Among other changes, the rule would expand public charge determinations to include an applicant’s enrollment in the Medicaid program. Adding Medicaid to the list of public charge benefits that would be considered may force immigrants to choose between health insurance coverage and a future green card—with adverse consequences for parents and their children.
Authored by: Emily M. Johnston, Genevieve M. Kenney, and Jennifer M. Haley for The Urban Institute
Topics: Affordable Care Act, Health, Housing, Immigrants, Legislation & Policy, Medicaid / Medicare, Safety
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Dec 6, 2018
Emily M. Johnston, Genevieve M. Kenney, and Jennifer M. Haley for The Urban Institute
The administration has proposed an expansion of the “public charge” rule that would make it more difficult for applicants whom officials deem likely to rely on public assistance to obtain lawful permanent residence (a “green card”) or a temporary visa.
0
Policy Brief
Community:
Dec 3, 2018
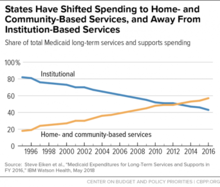
Some seniors and people with disabilities receiving home- and community-based services (HCBS) could lose their Medicaid eligibility and have to go into nursing homes to get needed care if Congress adjourns without extending “spousal impoverishment” protections that are set to expire on December 31.
Authored by: Judith Solomon for The Center on Budget and Policy Priorities
Topics: Affordable Care Act, Disabilities, Legislation & Policy, Medicaid / Medicare, Seniors
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Dec 3, 2018
Judith Solomon for The Center on Budget and Policy Priorities
Some seniors and people with disabilities receiving home- and community-based services (HCBS) could lose their Medicaid eligibility and have to go into nursing homes to get needed care if Congress adjourns without extending “spousal impoverishment” protections that are set to expire on December 31.
0
Publication
Community:
Nov 30, 2018
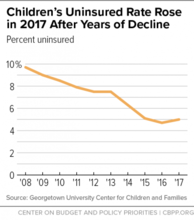
The uninsured rate among children rose in 2017 from 4.7 percent to 5 percent, a new report from Georgetown University’s Center for Children and Families finds — the first increase since Georgetown began producing this annual report a decade ago.
Authored by: Jesse Cross-Call for Center on Budget and Policy Priorities
Topics: Affordable Care Act, Child welfare, Health, Low-income, Medicaid / Medicare, Research
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Nov 30, 2018
Jesse Cross-Call for Center on Budget and Policy Priorities
The uninsured rate among children rose in 2017 from 4.7 percent to 5 percent, a new report from Georgetown University’s Center for Children and Families finds — the first increase since Georgetown began producing this annual report a decade ago.
0
Webinar
Community:
Jul 13, 2017
For providers in the Supportive Housing arena, it is no secret that the road to recovery begins with housing. However, this fact has not always been recognized by major healthcare entities, like Medicaid. Thankfully, this mindset is changing and Supportive Housing organizations now have the ability to cover many of their services via Medicaid. Since the rules and requirements vary tremendously state-to-state, many providers feel overwhelmed with the documentation required to bill Medicaid.
During this session, Foothold Technology and experts from various states across the country, including Steve Coe, CEO of Community Access, Kevin Martone, Executive Director of the Technical Assistance Collaborative, and Lindsay Casale, Housing First Program Director, Pathways Vermont, discuss the ins and outs of Medicaid for Supportive Housing. You will walk away with knowledge on: best practices from agencies already receiving Medicaid dollars; what reporting requirements providers should be aware of and on the lookout for, and how these can vary state-to-state; and tips on documentation methods and why a solid electronic record is crucial for Medicaid reimbursement.
For more supportive housing resources, join our online community at:
http://shrc.footholdtechnology.com/
Authored by: Foothold Technology
Topics: Affordable Care Act, Dual-eligibles, Health, Low-income, Medicaid / Medicare, Supportive housing
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Nov 14, 2018
For providers in the Supportive Housing arena, it is no secret that the road to recovery begins with housing. However, this fact has not always been recognized by major healthcare entities, like Medicaid.
0
Webinar
Community:
Nov 14, 2018
In the first session of this series, Foothold Technology Director of Client Services, Paul Rossi and Senior Advisor, David Bucciferro, along with Sue Augustus from CSH, bring us back to basics of all things Medicaid. They cover topics ranging in commonly used terms, coverage and eligibility and the differences between Medicaid and Medicare. This webinar series is designed for beginners and experts alike. Beginners will walk away with a strong foundation and experts will have the opportunity to contribute to the conversation.
Authored by: Foothold Technology and CSH
Topics: Affordable Care Act, Disabilities, Health, Low-income, Medicaid / Medicare
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Nov 14, 2018
Foothold Technology and CSH
In the first session of this series, Foothold Technology Director of Client Services, Paul Rossi and Senior Advisor, David Bucciferro, along with Sue Augustus from CSH, bring us back to basics of all things Medicaid.
0
Policy Brief
Community:
Nov 2, 2018
The new opioid legislation—the Substance Use-Disorder Prevention That Promotes Opioid Recovery and Treatment for Patients and Communities Act (the SUPPORT Act)—signed into law on October 24 includes targeted expansions in treatment, including provisions that provide funding or flexibility to states to expand access to treatment for substance use disorders (SUD), including opioid use disorder (OUD), and health care more generally in Medicaid and Medicare.
Authored by: Eva H. Allen and Lisa Clemans-Cope for The Urban Institute
Topics: Affordable Care Act, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Safety, Substance abuse
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Nov 5, 2018
Eva H. Allen and Lisa Clemans-Cope for The Urban Institute
The new opioid legislation—the Substance Use-Disorder Prevention That Promotes Opioid Recovery and Treatment for Patients and Communities Act (the SUPPORT Act)—signed into law on October 24 includes targeted expansions in treatment, including provisions that provide funding or flexibility to states
0
News Article
Community:
Sep 21, 2018
A children’s hospital in Columbus, Ohio, is trying to treat a difficult patient: Its own struggling neighborhood.
Authored by: Laura Bliss for CityLab
Topics: Affordable Care Act, Child welfare, Health, Housing, Low-income, Midwest, Partnerships
 Shared by Mica O'Brien
Shared by Mica O'Brien
Mica O'Brien posted a
on Sep 25, 2018
A children’s hospital in Columbus, Ohio, is trying to treat a difficult patient: Its own struggling neighborhood.
0
Report
Community:
Aug 9, 2018
UnitedHealthcare provides health insurance benefits to more than 40 million people across the country. In the past decade, it has addressed housing as a social determinant of health at the national level through policy leadership and financial investments, and at the state level working with local communities to connect Medicaid participants to stable housing. Through this work, UnitedHealthcare has overcome a myriad of challenges associated with siloed health and housing fields at all levels of policy and implementation. This case study explores how this national health payer has integrated the housing needs of underserved populations into its strategic priorities for investment and programming.
Authored by:
Topics: Affordable Care Act, Data sharing, Funding, Health, Homelessness, Housing, Low-income, Medicaid / Medicare, Partnerships
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Aug 9, 2018
UnitedHealthcare provides health insurance benefits to more than 40 million people across the country.
0
Policy Brief
Community:
Aug 9, 2018
Social determinants of health are the economic and social conditions that affect health outcomes and are the underlying, contributing factors of health inequities. Examples include housing, educational attainment, employment and the environment.
Authored by:
Topics: Affordable Care Act, Disabilities, Health, Homelessness, Housing, Low-income, Medicaid / Medicare, Mental health, Partnerships, Place-based, Substance abuse, Supportive housing
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Aug 9, 2018
Social determinants of health are the economic and social conditions that affect health outcomes and are the underlying, contributing factors of health inequities. Examples include housing, educational attainment, employment and the environment.
0
Case study
Community:
Aug 9, 2018
Health care payment and delivery models that challenge providers to be accountable for outcomes have fueled interest in community-level partnerships that address the behavioral, social, and economic determinants of health.We describe how Hennepin Health—a county-based safety-net accountable care organization in Minnesota—has forged such a partnership to redesign the health care workforce and improve the coordination of the physical, behavioral, social, and economic dimensions of care for an expanded community of Medicaid beneficiaries.
Authored by:
Topics: Affordable Care Act, Cost effectiveness, Health, Low-income, Medicaid / Medicare, Mental health, Metrics, Partnerships, Research
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Aug 9, 2018
Health care payment and delivery models that challenge providers to be accountable for outcomes have fueled interest in community-level partnerships that address the behavioral, social, and economic determinants of health.We describe how Hennepin Health—a county-based safety-net accountable care org
0
Publication
Community:
Jul 27, 2018
Anthem’s affiliated health plans and other managed care organizations (MCOs) increasingly are helping Medicaid members who are diagnosed with mental health conditions and substance use disorders (MH/SUD) find stable housing, secure meaningful employment, and address a range of financial and daily life challenges.
Authored by:
Topics: Affordable Care Act, Cost effectiveness, Depression, Funding, Health, Housing, Medicaid / Medicare, Mental health, Nutrition, Substance abuse, Supportive housing, Workforce development
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 27, 2018
Anthem’s affiliated health plans and other managed care organizations (MCOs) increasingly are helping Medicaid members who are diagnosed with mental health conditions and substance use disorders (MH/SUD) find stable housing, secure meaningful employment, and address a range of financial and daily li
0
Publication
Community:
Jul 27, 2018
On January 1, 2014, in states that have chosen to expand Medicaid eligibility under the Affordable Care Act, nearly all chronically homeless people who lacked health insurance became eligible for Medicaid. This Primer offers state Medicaid officials and other interested parties strategies for using Medicaid to meet the needs of this very vulnerable population--some strategies that have succeeded in the past and some that are emerging under provisions of the Affordable Care Act.
Authored by:
Topics: Affordable Care Act, Criminal justice, Disabilities, Dual-eligibles, Funding, Health, Homelessness, Housing, Low-income, Medicaid / Medicare, Mental health, Partnerships, Stability, Substance abuse, Supportive housing
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 27, 2018
On January 1, 2014, in states that have chosen to expand Medicaid eligibility under the Affordable Care Act, nearly all chronically homeless people who lacked health insurance became eligible for Medicaid.
0
Report
Community:
Jul 23, 2018
The aim of the study was to understand how policy capacity was defined and managed by state health leaders in different political environments during the implementation of the ACA. We conducted a total of 24 interviews, 18 with state executive agency officials and six with legislators from 10 states. The the final sample includes two states from the Northeast, three from the South, three from the Midwest, and two from the West.
Authored by:
Topics: Affordable Care Act, Funding, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Partnerships
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 23, 2018
The aim of the study was to understand how policy capacity was defined and managed by state health leaders in different political environments during the implementation of the ACA.
0
Report
Community:
Jul 23, 2018
The aim of the study was to understand how policy capacity was defined and managed by state health leaders in different political environments during the implementation of the ACA. Working with a sample of states—large and small, red and blue, actively reformist or more circumspect, etc.—the research team interviewed 18 state executive agency officials and six legislators from 10 states about their experiences developing and sustaining the capacity needed for major transformations in health care
Authored by:
Topics: Affordable Care Act, Funding, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Partnerships, Research
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 23, 2018
The aim of the study was to understand how policy capacity was defined and managed by state health leaders in different political environments during the implementation of the ACA.
0
Policy Brief
Community:
Jul 20, 2018
This report examines several ways in which health care changes created by the ACA, and other health care reform initiatives, create the potential for affordable housing providers to collaborate with health care providers, insurers, and other institutions to support the wellbeing of low-income individuals and families.
Authored by:
Topics: Affordable Care Act, Health, Homelessness, Housing, Legislation & Policy, Low-income, Medicaid / Medicare, Partnerships
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 20, 2018
This report examines several ways in which health care changes created by the ACA, and other health care reform initiatives, create the potential for affordable housing providers to collaborate with health care providers, insurers, and other institutions to support the wellbeing of low-income indiv
0
Research
Community:
Jul 19, 2018
The link between federal housing policy and public health has been understood since the nineteenth century, when housing activists first sought to abolish slums and create healthful environments. This article describes how the Obama administration—building on these efforts and those that followed, including the Great Society programs of President Lyndon Johnson—has adopted a cross-sector approach that takes health considerations into account when formulating housing and community development policy. The federal Department of Housing and Urban Development fully embraces this “health in all policies” approach. Nonetheless, the administration’s strategy faces challenges, including fiscal and political ones. Some of these challenges may be overcome by conducting quality research on how housing and community development policies affect health outcomes, and by developing a federal budget strategy that takes into account how investments in one sector contribute to cost savings in another.
Authored by:
Topics: Affordable Care Act, Community development, Disabilities, Health, Healthy homes, Housing, Legislation & Policy, Low-income, Mobility, Partnerships, Place-based, RAD, Research
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 19, 2018
The link between federal housing policy and public health has been understood since the nineteenth century, when housing activists first sought to abolish slums and create healthful environments.
0
Policy Brief
Community:
Jul 17, 2018
Medicaid is the nation’s public health insurance program for people with low income. The Medicaid program covers more than 70 million Americans, or 1 in 5, including many with complex and costly needs for care. The vast majority of Medicaid enrollees lack access to other affordable health insurance. Medicaid covers a broad array of health services and limits enrollee out-of-pocket costs. The program is also the principal source of long-term care coverage for Americans. As the nation’s single largest insurer, Medicaid provides significant financing for hospitals, community health centers, physicians, and nursing homes, and jobs in the health care sector. The Medicaid program finances over 16% of all personal health care spending in the U.S.
Authored by:
Topics: Affordable Care Act, Funding, Health, Legislation & Policy, Low-income, Medicaid / Medicare
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 17, 2018
Medicaid is the nation’s public health insurance program for people with low income. The Medicaid program covers more than 70 million Americans, or 1 in 5, including many with complex and costly needs for care.
0
Publication
Community:
Jul 13, 2018
This guide is organized around five steps, each of which includes concrete ways to get started as well as links to additional resources. These five steps will help you build a case for why and how Medicaid can be structured at the state and local levels to pay for services in permanent supportive housing. When building a case you need to know some basics of Medicaid and the types of services you want Medicaid to cover. in order to convince Medicaid administrators and other health care payers to support your efforts, you need to have evidence of need for and impact of supportive housing and you need a coalition of many stakeholders at your side.
Authored by:
Topics: Affordable Care Act, Data sharing, Funding, Health, Homelessness, Medicaid / Medicare, Partnerships, Supportive housing
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 13, 2018
This guide is organized around five steps, each of which includes concrete ways to get started as well as links to additional resources.
0
Policy Brief
Community:
Jul 13, 2018
A Toolkit for State Agencies
Authored by:
Topics: Affordable Care Act, Health, Legislation & Policy, Low-income, Medicaid / Medicare
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 13, 2018
A Toolkit for State Agencies
0
Report
Community:
Jul 12, 2018
Considerations for Mental Health and Substance Use Providers
Authored by:
Topics: Affordable Care Act, Health, Healthy homes, Legislation & Policy, Low-income, Medicaid / Medicare, Partnerships
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 12, 2018
Considerations for Mental Health and Substance Use Providers
0
Research
Community:
Jul 12, 2018
To construct our taxonomy, we use data from the first National Survey of ACOs, fielded between October of 2012 and May of 2013. The survey sample included (1) ACOs participating in Medicare ACO programs; (2) ACOs participating in state Medicaid ACO programs; and (3) ACOs formed in partnership with commercial payers.
Authored by:
Topics: Affordable Care Act, Medicaid / Medicare, Metrics, Research
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 12, 2018
To construct our taxonomy, we use data from the first National Survey of ACOs, fielded between October of 2012 and May of 2013.
0
Report
Community:
Jul 11, 2018
The 2017 edition of the Commonwealth Fund Scorecard on State Health System Performance finds that nearly all state health systems improved on a broad array of health indicators between 2013 and 2015. During this period, which coincides with implementation of the Affordable Care Act’s major coverage expansions, uninsured rates dropped and more people were able to access needed care, particularly those in states that expanded their Medicaid programs. On a less positive note, between 2011–12 and 2013–14, premature death rates rose slightly following a long decline. The Scorecard points to a constant give-and-take in efforts to improve health and health care, reminding us that there is still more to be done.
Authored by:
Topics: Affordable Care Act, Cost effectiveness, Health, Legislation & Policy, Low-income, Medicaid / Medicare, Preventative care, Racial inequalities, Research
 Shared by Housing Is
Shared by Housing Is
Housing Is posted a
on Jul 11, 2018
The 2017 edition of the Commonwealth Fund Scorecard on State Health System Performance finds that nearly all state health systems improved on a broad array of health indicators between 2013 and 2015.
 Shared by Housing Is
on Dec 11, 2018
Shared by Housing Is
on Dec 11, 2018




 Shared by Housing Is
on Aug 9, 2018
Shared by Housing Is
on Aug 9, 2018
 Shared by Housing Is
on Aug 9, 2018
Shared by Housing Is
on Aug 9, 2018
 Shared by Housing Is
on Aug 9, 2018
Shared by Housing Is
on Aug 9, 2018
 Shared by Housing Is
on Jul 27, 2018
Shared by Housing Is
on Jul 27, 2018
 Shared by Housing Is
on Jul 27, 2018
Shared by Housing Is
on Jul 27, 2018
 Shared by Housing Is
on Jul 23, 2018
Shared by Housing Is
on Jul 23, 2018
 Shared by Housing Is
on Jul 23, 2018
Shared by Housing Is
on Jul 23, 2018
 Shared by Housing Is
on Jul 20, 2018
Shared by Housing Is
on Jul 20, 2018
 Shared by Housing Is
on Jul 19, 2018
Shared by Housing Is
on Jul 19, 2018
 Shared by Housing Is
on Jul 17, 2018
Shared by Housing Is
on Jul 17, 2018
 Shared by Housing Is
on Jul 13, 2018
Shared by Housing Is
on Jul 13, 2018
 Shared by Housing Is
on Jul 13, 2018
Shared by Housing Is
on Jul 13, 2018
 Shared by Housing Is
on Jul 12, 2018
Shared by Housing Is
on Jul 12, 2018
 Shared by Housing Is
on Jul 12, 2018
Shared by Housing Is
on Jul 12, 2018
 Shared by Housing Is
on Jul 11, 2018
Shared by Housing Is
on Jul 11, 2018


















